Related Articles
Insights
Is Your Over-Reliance on Self-Reflection Hurting Your Team?
Leaders have become too focused on internal reflection at the expense of communicating effectively with others. In order to truly focus on a single target—such as a personal or team goal – you have to sacrifice your attention to other priorities.
Insights
Three Things to Do to Improve M&A Outcomes
Organizations face many challenges as they undergo mergers and/or acquisitions. Case studies of McChrystal Group's work with such organizations provide three key actions leaders should take to improve M&A outcomes.

Insights
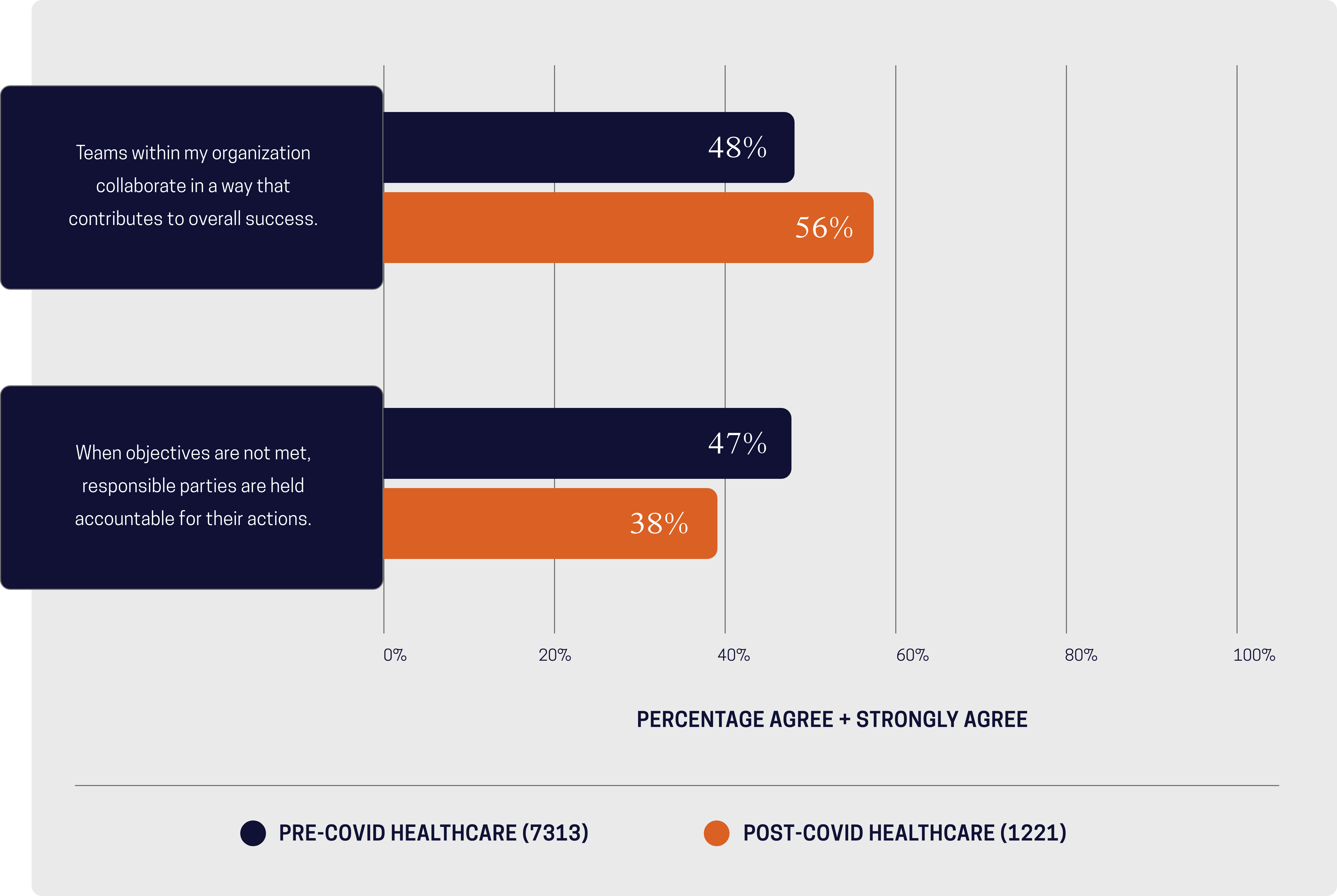
Healthcare – How do we prioritize when everything is a priority?
Healthcare and life science organizations remain steadfast in their mission – caring for and improving the lives of patients, but over time healthcare delivery has evolved. A growing set of complex objectives results in a plethora of services, programs, and technologies, layered one on top of the other, creating an avalanche of competing priorities. So how do we prioritize when everything is a priority?